A longtime leader in healthcare improvement, we’re developing new ways to revolutionize the industry.

It’s Flu Season: How Can Providers Improve Vaccination Rates Among Older Adults?
With the COVID-19 pandemic and life in general, it could be easy to miss that influenza (flu) season is upon us. Flu cases tend to increase in October, most commonly peak in February and last into May. According to the Centers for Disease Control and Prevention (CDC), last year’s flu season was light due to mask mandates and social distancing, which has some researchers predicting the flu could come roaring back.
As hospitals and health systems work through another round of COVID-19 and a severe flu season, how do providers increase flu vaccination rates to keep communities healthy? For starters, providers and other experts are recommending that people of all ages get their flu vaccines now. Researchers have indicated that if there is an increase in the number of Americans getting vaccinated, then we could avoid a severe flu season altogether.
But which flu vaccine should patients receive? How can providers educate patients about their options, overcome patient vaccine hesitancy, reduce racial and ethnic disparities and ensure supply to increase flu vaccination rates?
PINC AI™ Applied Sciences (PAS) and Sanofi Pasteur are Helping Providers Develop a Process
PAS is embarking on a quality improvement research project, funded by Sanofi Pasteur, to explore what provider, system or patient characteristics are identified by clinicians as barriers and facilitators to flu vaccination rates in adults age 50 and older and higher-risk populations. In addition, the project studies what quality improvement approaches can help to overcome these barriers and improve flu vaccination rates in those populations.
During this eight-month project, the team aims to help providers understand the benefits of using FDA-approved influenza vaccines in adults over the age of 50, including high-dose vaccines. Higher-dose vaccines are defined by the amount of hemagglutinin antigen that the vaccine delivers. Older adults may have weaker immunogenic responses to standard flu vaccination compared to younger adults and their antibody levels may decline more quickly. This project will assess and address the needs for older adults to receive the most effective influenza vaccination available.
To conduct the research, the PAS team first set out to capture and evaluate provider perceptions and insights regarding barriers to flu vaccinations. They aim to work with providers to develop strategies and action steps to:
- Identify patients eligible for high-dose flu vaccines.
- Educate patients about vaccination.
- Assess clinic processes to maximize vaccine administration.
They identified primary care clinics at two Premier health system members, Centura Health System and Texas Health Resources, that agreed to engage with the team to better understand their trends and gaps around flu vaccination rates.
“Participating in this study has helped us become more aware of our flu vaccine ordering patterns,” said David Alvarez, Clinical and Ambulatory Care Pharmacist at Centura Health. “This effort has helped us establish a standard process for evaluating our patient population and understanding our standard flu and higher-dose flu vaccine needs.”
The team has instituted peer-to-peer learning calls and discussions about perceptions of barriers to vaccination, and best practices that could benefit from improvement efforts. They used Premier’s Custom Intervention Platform (CIP) to securely capture and display patients eligible for flu vaccines and a measures dashboard shows rates of flu vaccine administration.
Supply and Demand: Finding the Balance
The team is also working with primary care clinics to better understand their flu vaccine ordering processes. Health systems typically place their order for the next season’s flu vaccine as the current season comes to an end. Ideally, they base their order on the specific needs of their patient population, storage capacity and doses administered during the previous flu season.
This project has identified potential gaps in communication as the flu season approaches and progresses, where clinicians could be more informed and involved more regularly with ongoing stocking and vaccine choice decisions. Collaborative planning could prevent trade-offs between vaccine timing and administration of flu vaccine for those higher-risk patients.
When clinicians are more in tune with their populations and participate in the ordering process, they can increase and decrease their high-dose vaccine order throughout the flu season, ensuring they have enough supply of all vaccine options for all patients in their practices.
Ensuring Patients Understand Vaccine Options
People have always been reluctant to receive a shot of any kind, and rumors run rampant that you can get the flu from the vaccine, but that isn’t true. There is a zero percent chance of getting the flu from the flu shot since each shot is made from inactivated flu viruses, or with only a single protein from the flu virus. While the flu vaccine isn’t a 100 percent guarantee that people won’t get the flu, it does reduce the risk of infected patients having to go to the doctor by 40-60 percent.
To compound the problem, some people have become hesitant about visiting the doctor because of the COVID-19 pandemic. Some are also hesitant about newly introduced mRNA vaccines. Additionally, people have questions about whether they can or should get a flu and COVID-19 vaccine simultaneously. The CDC has stated that it is safe to get the flu and COVID-19 vaccine at the same time with an emphasis on the importance of getting vaccinated overall.
In addition to lack of vaccine education, there are concerning racial and ethnic disparities that saw 56 percent of white Americans getting vaccinated last flu season compared to 43 percent of Black Americans and 45 percent of Hispanic Americans.
Clinicians should share their flu vaccine process with patients and provide education regarding the flu vaccine options for each age range. This allows patients the chance to make the most educated decision on the right flu vaccine for them and address their health concerns surrounding the vaccine.
Developing a Plan
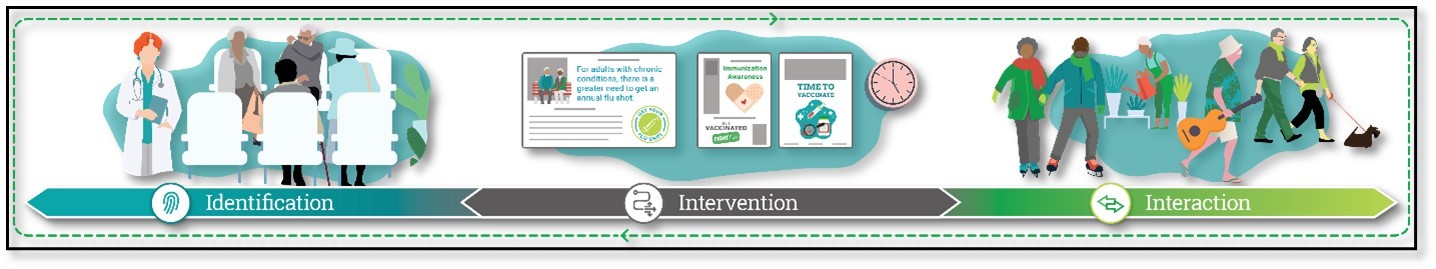
PAS is using the 3Is Framework™, a tool they developed, that helps design rapid cycle changes to close gaps in care. The Framework will help providers develop a sustainable process for identifying eligible flu vaccine patients, helping providers intervene with education around the importance of vaccination and assist providers in interacting with their patients to help them overcome hesitancies related to vaccines.
PAS has worked to offer research, real-world data and evidence for more than 20 years. As experts in implementation science, the team takes a strategic, collaborative and customized approach to identifying barriers to implementing best practices and finding interventions that can accelerate adoption and interaction of all stakeholders at the local and system level.
With this project, the team is working to help develop protocols and sustainable solutions that can be scaled nationally to improve flu vaccination rates for all patients and specifically patients age 50 years or older.
These improvements to processes should help get more people vaccinated to prevent cases of the flu and decrease transmission. Evidence has shown that influenza can kill anywhere between 12,000 and 52,000 people a year, depending on the flu season, and puts as many as 700,000 people in the hospital. Increasing vaccination rates among all patients can help keep a flu surge at bay, especially as hospitals and providers struggle to cope with surges caused by COVID-19 variants.
From these process changes, supply chain improvements and patient engagement strategies, it’s clear that any small changes could have a huge impact.
Get more details on this year’s flu season with these safety resources.
Learn more about PINC AI Applied Sciences and PINC AI™ Healthcare Data.
The insights you need to stay ahead in healthcare: Subscribe to Premier’s Power Rankings newsletter and get our experts’ original content delivered to your inbox once a month.

